While there’s no cure for hidradenitis suppurativa, experts are testing new treatments. Some provide relief from painful abscesses that drain pus and scar the skin.
HS isn’t caused by poor hygiene, and it’s not contagious. The cause is unknown, but genes and hormones play a role.
Managing HS requires lifestyle changes. You’ll likely see a healthcare provider who specializes in skin diseases called a dermatologist.
Identify Your Symptoms
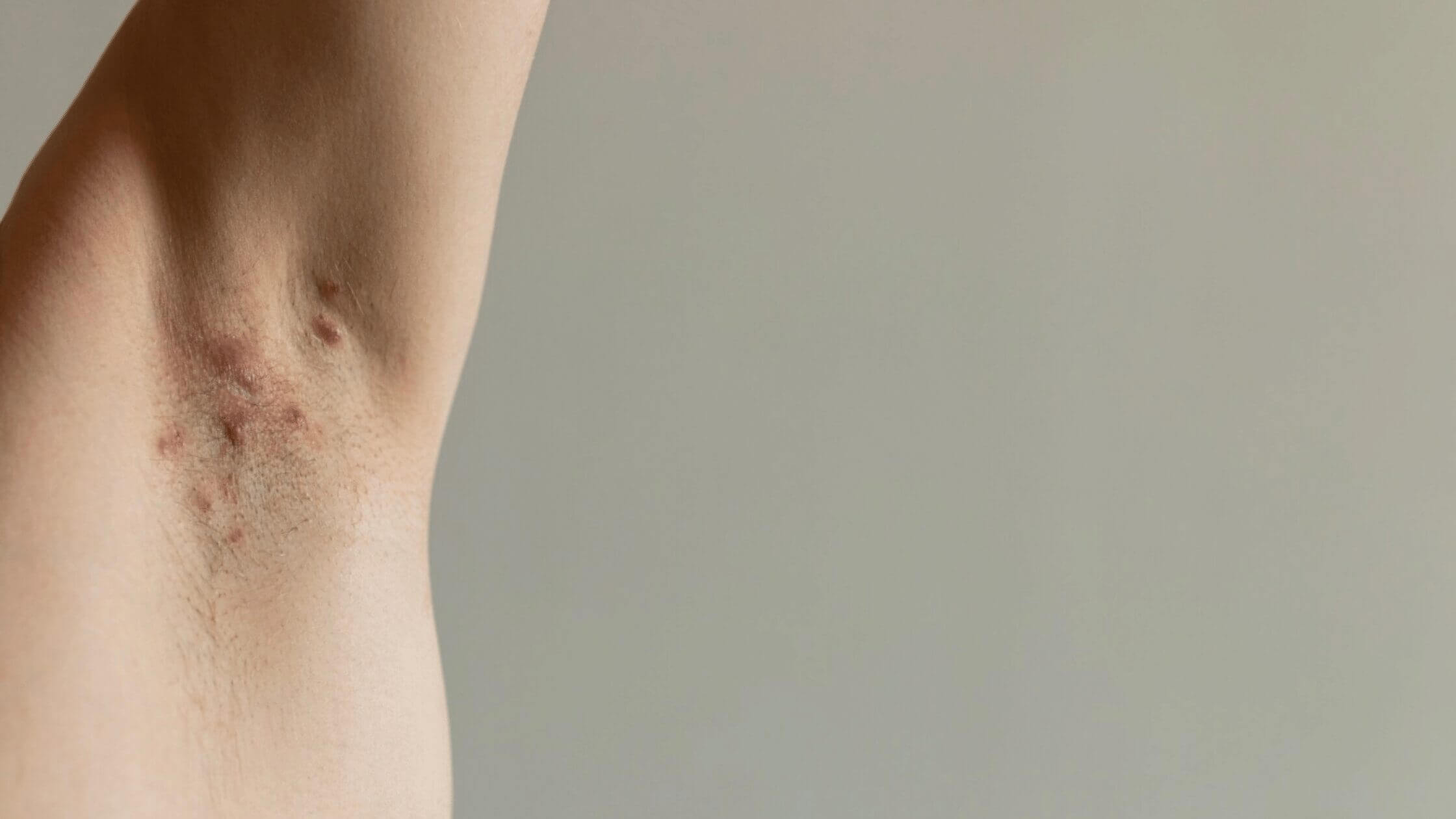
Hidradenitis suppurativa causes boils, or pockets of infection (abscesses), in the armpits and genital area. It affects women more than men, and it may run in families. The condition is not caused by poor hygiene and is not contagious.
The first step is to see your healthcare provider. Your healthcare provider will base a diagnosis on your symptoms, skin appearance, and medical history. They might refer you to a healthcare provider or dermatologist specializing in skin diseases. You might also be referred to a specialist in colorectal surgery, plastic surgery, or gastroenterology.
Your doctor will want to know what makes your hidradenitis suppurativa worse or better. You might tell them if the pain and swelling improve when you wear loose clothing or if it gets worse with certain foods.
Your doctor might prescribe antiseptic soap to wash your affected skin daily and to clean the areas where abscesses occur. You might be given a sterile absorbent dressing to put over the wounds and change them at least once daily. You might also be prescribed a topical medication to ease the inflammation and stop infections from growing in the abscesses.
Take Care of Your Wounds
Many people with HS feel stressed, depressed and anxious about the condition. Contact friends and family for support or seek professional help if you feel down. You could also join a support group for people with the same situation.
Some at-home and prescription treatments can reduce pain, ease inflammation, prevent boils from forming and thwart infections that arise when boils burst. A skincare routine that includes gentle washing, wearing looser clothing, weight loss and avoiding trigger foods can make you feel better.
Hormonal therapy might be helpful for some people with mild hidradenitis suppurativa. Medications such as the oral contraceptives spironolactone and metformin might help, especially during premenstrual flare-ups. And isotretinoin, a drug that treats acne, might reduce your need for antibiotics and lessen the severity of outbreaks.
Infliximab and adalimumab are immunosuppressive drugs that might be useful for moderate to severe cases of hidradenitis suppurativa. They are given as injections at home or in the hospital and might be used in combination with other treatment options. These medications have serious side effects and are not recommended if you’re pregnant or breastfeeding.
Take Control of Your Diet
Hidradenitis suppurativa can cause painful sores that drain pus and leave a foul odor. These sores often develop where skin rubs together, such as the armpits or groin. Hidradenitis suppurativa most commonly occurs after puberty and seems linked to hormones. But despite its unpleasant appearance, this condition is not contagious.
Although there is no cure for HS, there are treatments that can significantly improve your symptoms and quality of life. Your doctor will recommend a treatment plan that may include antibiotics, which can be spread on the skin (topical) or taken by mouth, such as lymecycline, doxycycline or erythromycin. Antiseptic washes with 4% chlorhexidine also can help control infection. Retinoids, such as acitretin, which is vitamin A-based, are also used to help.
Experts are working to find new treatments and ways to prevent HS. For example, they explore using steroid shots directly into the sores to reduce inflammation. They might also suggest surgical removal of boils. This might involve removing all the affected skin and graft to close the wound in severe cases.
See Your Health Care Provider
There’s no cure for hidradenitis suppurativa, but treatment can help ease pain and reduce the number of boils. Gentle skin care, avoiding foods that trigger flare-ups and, for some people, a change in diet can all be part of a regimen to manage symptoms. If over-the-counter (OTC) medications don’t help, a healthcare provider might prescribe stronger ones. NSAIDs like aspirin (Aspirin should not be given to children due to Reye’s syndrome) and Motrin may relieve some pain. At the same time, antibiotics can treat bacterial infections that result when boils burst or leave open wounds.
Corticosteroid creams, pills and injections can reduce inflammation in the affected area. If boils are severe, your healthcare provider might drain them using an incision and drainage procedure. They might also expose tunnels under the skin to air, a process called unroofing, to prevent future boils. Other surgical procedures that might be needed include wide surgical excision, a system that removes all boil-like tissue and healthy surrounding tissue in the affected areas; punch debridement, which involves removing an individual boil; or fistula surgery, a procedure that creates a permanent connection between the skin and the bowel or bladder.
Stay Active
Getting treated for hidradenitis suppurative (HS) is important because it can help prevent complications, such as infection or scarring. But living with HS can also be difficult. It can make you want to avoid going out or joining in activities with friends, like group sports. It can even make you self-conscious about your skin and its appearance.
The condition can cause painful boils that sometimes drain or bleed. But you can do things to ease the pain and prevent flare-ups, such as taking an anti-inflammatory medication or topical cream. A variety of home remedies can help, too, such as a diet rich in zinc, which helps heal wounds and boost the immune system.
Hidradenitis suppurativa is usually concentrated in areas with many skin-to-skin contacts, such as the armpits and groin. These areas can chafe and hurt during activity. Getting enough sleep and eating well can also help. And if you do develop a rash, see your doctor right away. Some people may need comprehensive care from a healthcare team with doctors from different specialties.